Enjoying the great outdoors is so beneficial to our emotional and physical health. But how might those feel who’ve fallen victim to the effects of Lyme disease? We’re going to take a deep dive into this important topic. It seems the occurrence is on the rise, though that may well be due to better diagnostics. For many years, diagnosing this disease would prove to be quite difficult leading to missed or delayed treatment, leaving many victims suffering with the long-term effects of what can be a devastating disease. We would later learn that Lyme disease is much more prevalent than we’d ever thought. By drawing attention to this, especially as we anticipate spring, my hope is to promote knowledge of risks, protective measures, and early recognition of the condition with prompt diagnosis. We would also like to empower would-be victims to investigate various treatment modalities and advocate for themselves or their loved ones in a timely manner.
Lyme disease is the most common tick-borne illness in the United States and Europe. It was first discovered after what was thought to be an outbreak of juvenile rheumatoid arthritis in Lyme, Connecticut and surrounding communities. Since juvenile rheumatoid arthritis does not occur in outbreaks, researchers studied these patients, noting the characteristic rash. Eventually they identified the offending bacteria that causes what became known as Lyme disease.

Blacklegged or “deer tick”
Ticks are parasites, specifically arachnids, that attach to and feed on the blood of birds, reptiles, and mammals. Dogs are frequent hosts. Not all ticks carry or transmit Lyme disease.
Lyme disease is caused by the bacterium borrelia burgdorferi and is transmitted through the bite of infected blacklegged ticks, also known as deer ticks. Hunters often see ticks attached when skinning a deer. More prevalent in the Northeast and Midwest, Michigan is included in this target area.
According to the CDC, the percentage of deer ticks that carry the disease ranges anywhere from 2 to 50% based on the area of risk. Tick hot spots are located near available food and water, including property that borders forests where field mice are abundant. (A common host.) Though ticks do not jump, hop or fly, they sense warmth and carbon dioxide (CO2) given off by animals and humans, and latch themselves onto anything that brushes up against them. My husband would argue that another mode of travel for these parasites would be “riding on a wind current,” as he experienced one day when he actually saw ticks descending from a particularly high wood pile towards their intended targets, one of which was him! They may make their way up into trees by hitchhiking on birds, then free falling or seemingly floating towards CO2 producers, though ground birds would likely be a more common host. They can also be carried into the home on exposed clothing and later be found crawling up the wall, including that of the shower. Ticks are hard to kill with their tough outer shell. Jim, a friend of ours, who has dealt with chronic Lyme disease tells of experimenting on ticks after dragging a white towel around the yard in late spring as he collected a few this way. One lived in the bottom of a glass of water for a very long time. Another was still moving after spending several days in the freezer. He tried mosquito spray, but this did not seem to affect them in the least.
When we look at risk factors, outdoorsmen in general exist in the middle of this cesspool. Just playing outdoors risks exposure. Who can go on a walk in the woods or tall grasses without later finding a notorious tick on them? Hence the subtitle to this article… “Once bitten, twice shy.” Ticks take up to 24 hours from contact with skin before they actually start to feed on their host’s blood. Then they must remain firmly attached for 48 to 72 hours to pass the Lyme disease causing bacteria to humans, if that’s any consolation. The key is to remove the tick before it becomes engorged to minimize the risk of disease transmission, which is reduced to about 1 in 100 when this timely action is taken. The most common sites for tick bites are the armpits, groin, backs of the knees, or belt line. The back of the neck or scalp are more common in children. (And shorties, like me.)

An engorged tick removed minutes earlier & placed in a baby food jar.
Though particularly rampant in May and June, this past year, we encountered ticks in April, and even found a poppy seed sized tick in October. In early December my husband found an engorged tick embedded in his hip. We’re new to using a wood burning stove to augment our heat source. Ticks go dormant in the winter, but can become active during warm spells. Perhaps that would include during their inadvertent admittance into the home when they crash the party incognito amidst the firewood. One might begin to feel a bit of paranoia, or more like ‘arachnophobia’ about outdoor life. Though tick life abounds, there are measures that can be taken to minimize skin contact proactively, then perform the infamous “naked tick dance” after outdoor activity. Check out Brad Paisley’s song, “Ticks” if you’d like to put a more positive slant on this body scan… “I’d like to check you for ticks.”
Removal of ticks can be tricky, especially if the tick becomes embedded. The following illustration demonstrates using tweezers. Be sure to remove the entire tick with no parts left behind.
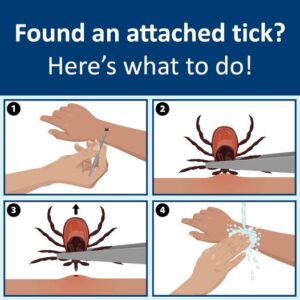
Jim’s personal preference for disposal of ticks is the hammer, adding an element of satisfaction. Taking protective measures when it comes to your clothing for outdoor activity can greatly reduce tick access. Light colored clothing will help to better identify ticks before they make their way to skin and attach. Be sure to tuck your pants into your boots. Some use permethrin, a synthetic insecticide made from chrysanthemum flowers that works by disrupting insect nerve cells causing paralysis and death. It comes as a spray for clothing (NOT SKIN), to help deter ticks, but directions must be followed and cautions acknowledged.

Check for ticks between toes, underside/belly, head neck & ears.
Just a reminder that your dog can carry ticks, which can affect his health and yours, so be sure to check your dog, too.
Dr. Renee Coyer, owner of Upper Peninsula Veterinary Service & ThunderPaws Boarding says there has been a steady upswing in ticks and thus the diseases they transmit over the past 10 years. “Ticks are a year round problem. There is no ‘safe’ season.” She says the first line of defense to prevent disease is for pet owners to check their dog for ticks, then remove and dispose of ticks to avoid future exposure. “The second line is using a veterinary approved product for protection.” Dr. Coyer emphasizes that not all products are equal for speed of kill or concentration over those 30 days. Over the counter products lack customer support. She urges pet owners NOT to purchase products from the internet which ‘guarantee’ to keep your pets safe, chemical free. She also says not to rely on herbal products as the exclusive means of protection for your pet. “Third line of defense is the use of Lyme Vaccination for both dogs and horses. Work together with your veterinarian to protect your 4 legged family from the year-round threat of tick borne disease.”

A classic “bulls eye” with white center
Symptoms of Lyme disease vary widely and may present in different stages of the infection. In the early stages (days to weeks after the bite), victims may note a red, expanding bull’s-eye rash (erythema migrans), fever, fatigue, headache, muscle and joint pain, and swollen lymph nodes. Without the bull’s-eye rash, a more obvious sign, these insidious symptoms mimic many other illnesses, such as influenza or other viruses. The tell-tale bullseye rash is only present in about 20-30% of Lyme cases. The Lyme rash is often mistaken for a spider bite, though typically, a spider bite does not expand in size. Tick bites from non-infected ticks are typically dime sized or smaller and do not expand in size. Bacteria from Lyme disease can get into the bloodstream and create other skin lesions distant from the site of the initial bite.
Weeks to months after the bite, second stage symptoms may include arthritis, (knees, ankles, etc.) neurological symptoms, like facial paralysis or meningitis, and heart problems, such as palpitations. Late stage (months to years after onset), one may experience chronic arthritis, cognitive impairment, mood changes, skin problems, and chronic fatigue. Again, these symptoms mimic many other conditions, so a proper and timely diagnosis is paramount.
For those who may be afflicted by Lyme disease, time is life, or at the very least, quality of life. We are our own best advocate for health. Unfortunately the health care system can be challenging to navigate. They’re much more up to speed on this disease than they were even just a few years ago. Still, if you’re not assertive, you can get lost in the shuffle, delaying treatment and negatively impacting the long term outcome. So where does one start if they suspect they may have Lyme disease? Typically, a blood test is done for diagnosis. The CDC recommends a two step testing process. Many cases of Lyme disease are initially misdiagnosed, as blood tests are not always dependable, particularly in early disease. There can be false positives and false negatives, which can be so frustrating to those experiencing symptoms of the disease. Jim experienced this early on as he struggled to get a definitive diagnosis in 2010 when he experienced many of the classic symptoms, though no rash. He tested negative initially and ran the gamut of seeing different specialists, from Cleveland Clinic, to U of M, Beverly Hills, MI, and eventually was referred to an MD that also practices alternative medicine in Grass Lake, who felt that CDC tests were not as sensitive for diagnosing. He sent Jim’s blood to a lab in Australia which showed up as positive for a specific strain of Lyme.
Fast forward to 2019 when our friend Nick was diagnosed. Knowledge has expanded on this topic and his health care provider immediately ordered a boat load of lab work, which thankfully included screening for Lyme disease despite the lack of a bullseye rash. Typical medical treatment includes 10 to 14 days of antibiotics for the early stage. The timing and duration for antibiotics varies based on symptoms and stage of disease. This may be given orally or intravenously depending on severity. For Nick, with a prompt diagnosis, the antibiotic doxycycline was started, and based on the severity of his symptoms, was extended to a 30 day course. He had bad flu symptoms, very painful widespread aching and was also placed on steroids. It took a full year for him to feel like his old self, but in the meantime, experienced bouts of extreme pain for which the narcotic, Norco was ordered. He often took ibuprofen to help cope and applied Icy Hot to affected areas to provide some relief. He avoided the Norco due to the risk of addiction. It can also affect one’s mental state. Though he did not go on disability from work, he recalls burning up a lot of his earned time off when the condition became intolerable.
Even after treatment, some people experience lingering symptoms, a condition known as post treatment Lyme disease syndrome (PTLDS). Antibiotics are often effective for fast growing bacteria, however, borrelia burgdorferi is a slow growing bacteria. Prolonged antibiotic use can create antibiotic resistance and can also destroy healthy bacteria in the gut and skin which are essential to the functioning of our immune system and decreasing inflammation throughout our bodies. Other medications used to treat symptoms may also have negative side effects that impact general health, namely gut health, though other organs can be affected.
Our friend, Jim, is still affected by PTLDS, having good days and bad days. He says he basically “got older faster.” For a time he experienced visible muscle twitching to his eyelids, abdomen and legs. Along the way he was suspected to have superimposed Cytomegalovirus for which he was placed on antiviral medication that greatly decreased his liver function before the medication was discontinued. He later had a tick bite that actually developed the classic bullseye rash, and went through another cycle of antibiotics. Jim was placed on disability from his job at one point, recovered to a functional level, after which he returned to work, though never feeling completely back to his prior state. PTLDS led to an earlier retirement than he’d planned on, having retired in 2019. He still has periods of extreme exhaustion, this becoming a part of his new normal.
Some have had better success using a holistic approach, such as herbal therapy and nutritional support, namely an anti-inflammatory diet. There is also the option of combining conventional therapy with holistic care. Jim followed Dr. Bill Rawl’s treatment protocol, seeing some improvement that then seemed to level off. Nick was grateful that his MD was very open to complementing his medical care with holistic care. Nick was initially a skeptic, referring to his holistic provider as his “voodoo doctor,” (through Hummingbird Health in Harbor Springs) but in the end credits this aspect of care as being the key to his recovery. He was placed on various herbal remedies and essential oils to strengthen his immune system and promote gut health as he fought off this disease. He still experiences occasional flare ups, specifically intense body aches. Nick stated that his biggest challenge when he gets sick or has a set back is that his recovery time takes longer than pre-Lyme, being exhausted and sore for longer periods of time in relation to any illness.
The financial burden of treatment creates additional stress for many, especially for those seeking non traditional treatment modalities. Even the cost of finding a diagnosis in the face of false negatives, and insurance companies not wanting to pay for further testing, can be overwhelming. For those experiencing PTLDS, this challenge is magnified based on the prolonged nature of treatment. As the number of cases grows, we can only hope for more accurate diagnostics and effective treatment options and that these will be well recognized and covered by health insurance companies. In the meantime, perhaps it would be a good idea to contact our governmental representatives regarding this important health issue.
Let’s consider one more thing, and that’s our general health. Building a strong immune system begins with a healthy gut microbiome, which healthy eating contributes to. Moderate exercise, fresh air, sunlight, and adequate sleep are essential for optimal health. Being healthy before illness will allow the body to better respond to any stress it encounters, including Lyme disease.
**********
*I’d like to thank Jim Kushner and Nick Breed for contributing to this article by sharing information from their own personal journeys.
*I’d also like to thank Dr. Renee Coyer, DVM, for providing information from a veterinarian perspective.
References:
Johns Hopkins University Medicine Research Center website
Dr. Bill Rawls, MD
Linden Hu, MD Lyme Disease Prevention and Treatment, American Society for Microbiology
Images used from CDC.gov and MDHHS at michigan.gov
- THE ICE STORM OF ‘25-ONE YEAR LATER- - March 21, 2026
- THE LONG WINTER AND NATURE’S CONSEQUENCES - March 21, 2026
- TICKS AND LYME DISEASE – “Once Bitten, Twice Shy” - March 6, 2026

